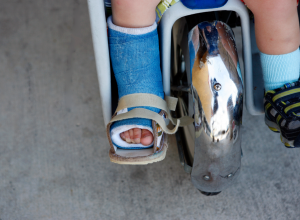
Clubfoot
Clubfoot, also called talipes equinovarus, is a deformity in which an infant is born with one or both feet in an unusual position, usually inward or sideways. It is one of the most common foot deformities seen in newborns, happening in about one in 1,000 births. Clubfoot is a painless deformity, but it must be treated soon after birth to prevent walking problems later on. With proper treatment, most children with the condition grow to enjoy normal physical activity with little to no sign of the foot deformity.
Symptoms
Most cases of clubfoot are present at birth, meaning it is congenital. The condition is painless in infancy, whether the deformity is mild or severe. Most all cases of clubfoot share the following characteristics:
- One or both feet are turned inward or downward
- There is a deep crease on the bottom (sole) of the foot
- The foot and legs are shorter than normal
- The calf may be thinner and underdeveloped
Clubfoot will not improve on its own. If left untreated, the condition may lead to your child having difficulties walking, severe calluses, lifelong pain and the inability to wear shoes.
Causes
Clubbed feet develop when the tendons that connect your child’s leg muscles to his or her foot bones are unusually short and/or tight. This causes the foot to twist inward and upward or downward. About half of all cases of clubfoot affect both feet.
Some cases of clubfoot are the result of the baby’s position in the womb (postural clubfoot), while others are caused by genetics. Infants have an increased risk of developing clubfoot if there is a history of the deformity in the family.
Experts aren’t sure why, but boys are twice as likely as girls to have clubfoot.
There are two types of clubfoot: isolated and nonisolated. Isolated appears in children who have no other medical issues, while nonisolated appears in combination with other health conditions, including neuromuscular disorders. Because of this, most children born with clubfoot are screened for other health conditions, including stroke and brain injury.
Treatment
It is extremely important that any infant born with clubfoot begins treatment with a foot doctor or orthopaedic surgeon right away. The condition will not improve on its own, and sites like WebMD, MedlinePlus, and MedScape all agree that a delay in treatment could lead to a permanent foot deformity that inhibits your child from walking, running and engaging in other types of physical activity.
Stretching and Casting
Most cases of clubfoot can be treated with conservative, non-surgical methods like stretching, casting and bracing. These methods are done daily for a period of several weeks to several years and help slowly move the foot into a normal position. There are three types of non-surgical manipulation that use gentle stretching and casting or taping to achieve gradual foot movement: traditional, Ponseti (Iowa) and French.
Traditional treatment uses a combination of gentle stretching and bracing to fix the foot one position at a time, usually starting with the inward direction of the foot being corrected first followed by moving the foot upward or downward.
The Ponseti treatment aims to fix two positions at a time, simultaneously bringing the foot outward as well as up or down. The Ponseti treatment is successful in about 90 to 100 percent of children born with the deformity and is the most common treatment used in the US.
French treatment incorporates initial stretching but follows up with taping rather rather that casting the foot. As with the other two methods, the French method requires daily manipulation of the foot followed by taping.
All the above methods may require one minor surgery to lengthen the Achilles tendon (heel cord). This surgery is called tenotomy, and it involves cutting the tendon so that it can regrow into a proper, longer length. The foot is re-cast after this procedure, usually for a period of about three weeks.
Nonisolated clubfoot that appears with conditions like spina bifida and arthogryposis generally require surgery and are typically much harder to heal than isolated conditions.
Bracing
Many cases of clubfoot will reoccur, so bracing is often suggested after several weeks or months of stretching and casting are completed. If a brace is required, your baby will typically start out wearing the brace full time (22 to 24 hours per day) and then will gradually decrease to wearing it during the night and nap time only (about 12 hours per day). Your baby may need to wear the brace (usually called a boots and bar, Denis Browne bar or Ponseti AFO) for several years to ensure that the foot stays in its newly corrected position.
Babies are generally resistant to wearing the brace and may be fussy for the first few days. However, most will adjust and get used to the brace within a week or so. For more information, read our article Tips To Help Your Child Adjust To Foot and Leg Braces.
Surgical Treatment
While surgical treatment is rare, sometimes it is suggested for severe cases of clubfoot or for reoccurrences of clubfoot (which typical happen when parents do not fully follow the non-surgical treatment options). Due to overcorrection complications as well as future foot stiffness and pain, clubfoot surgery is always considered a last option.
If stretching and casting has already been done, then less extensive surgery is typically needed. These procedures usually involve cutting the Achilles tendon or moving the tendon (called an anterior tibial tendon transfer).
If major reconstructive surgery is done, it usually involves extensive release of tissue structures in the foot. The foot is then stabilized with pins and a long-leg cast until it heals, which typically takes about four to six weeks, followed by a short-leg cast for a period of about four weeks. This is then followed up with special shoes and/or bracing for a period of a year or longer.
What to Expect Long Term
As mentioned above, clubfoot will not heal on its own. However, with proper treatment that begins soon after birth, your child should grow to have a near normal foot and be able to engage in regular physical activity. Sometimes the affected foot is a size smaller and the calf muscles in that leg may be thinner, which can create slight leg pain. The pain is generally mild and does not create any further issues or problems.
Notice concerning medical entries:
Articles having medical content shall serve exclusively for the purpose of general information. Such articles are not suitable for any (self-) diagnosis and treatment of individual illnesses and medical indications. In particular, they cannot substitute for the examination, advice, or treatment by a licensed physician or pharmacist. No replies to any individual questions shall be effected through the articles.