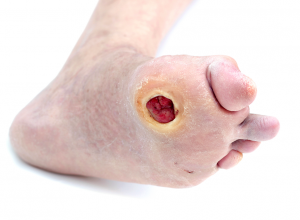
Charcot Foot
Charcot foot, also called Charcot arthropathy and Charcot neuroarthropathy, is one of the most critical foot conditions people with diabetes and other neuropathic conditions can develop. It is characterized by fractures and/or dislocation of bones and joints in the feet and ankles that a patient is unable to feel. Left untreated, this bone destruction quickly leads to deformation of the foot and possible disability.
Charcot foot was named after French neurologist Jean-Marie Charcot, who noticed a pattern of bone destruction in patients with tertiary syphilis and other conditions leading to a loss of sensation in 1868. William Jordan noticed a similar pattern in diabetic patients in 1936.
Causes
Charcot foot arises when a person cannot feel pain or other sensations in their feet — most always due to diabetes mellitus, loss of sensation, chronic aloholism or other neuropathic conditions — and suffers bone fractions or dislocations in the foot or ankle without realizing it. Continuing to walk on the foot results in more fractions and dislocations, some of which can be quite severe. In some cases, bits of broken bone begin to poke through the skin, which can cause chronic foot sores that are tough to heal and may never go away. In combination, the trauma can lead to a foot becoming warped and permanently deformed.
Theories as to what causes the bone fractures to begin with vary, but two predisposing factors seem to be common in those who develop Charcot foot: the patient suffers from peripheral sensory neuropathy or a total absence of sensation, and he or she has a history of preceding injury (most often so minor, the patient can’t recall it ever happening). Some patients also experience poor circulation, which has been linked to weakening of the bones.
Symptoms
The majority of people with Charcot foot do not feel any pain or sensation in their feet due to neuropathy (nerve damage). Therefore, the condition is most often noticed by appearance only. The most common initial sign of Charcot arthropathy is swelling of the foot. As the condition worsens, the skin might start to appear red, the foot could morph or change shape, and sores or ulcerations may start developing as bits of broken bone begin to pierce through the flesh. In addition, the involved joints will show signs of crepitus (a grating or grinding that happens as a result of bone and cartilage rubbing together).
Charcot foot is often misdiagnosed. The swelling and redness can be mistaken for a bone infection, cellulitis, gout, osteomyelitis and tendonitis.
Treatment
Treatment for Charcot foot involves first healing the bones and then preventing further or future foot deformity. Because the condition worsens quickly, early diagnosis is critical.
Initial treatment of Charcot foot usually entails complete immobilization of the affected limb. This includes applying a cast or brace to the involved extremity as well as making sure it does not bear any weight. The duration of immobilization will depend on the severity of the condition and the joints affected, but it usually lasts three months or more.
When a doctor approves small increments of weightbearing, special shoes and/or orthoses may be necessary as the bones and joints continue to heal. Sometimes orthoses are recommended to help the patient avoid developing ulcerations. Foot sores often times resist conservative treatment and quickly become infected in patients with neuropathic conditions (due to poor circulation), meaning surgery is often required to prevent the loss of a limb.
Foot and ankle deformation stemming from Charcot foot is common, with midfoot collapse (“rocker-bottom”) being reported most often. If deformation is present, surgery is often required in order to prevent foot amputation.
Prevention
While there is no surefire way to prevent Charcot foot from developing, there are ways to lessen the degree in which the condition progresses. Patients who have been diagnosed with diabetes or other neuropathic conditions oftentimes cannot feel sensation in their feet, so they should be inspecting each foot on a daily basis for injuries, sores, ulcers, blisters, ingrown toenails, swelling, redness and any other sign of a problem. Noticing abnormalities early on and seeking treatment can prevent infections, further complications, and limb amputation.
For further information on diabetic foot care, check out our article Simple Steps to Prevent Diabetic Foot Problems.
Notice concerning medical entries:
Articles having medical content shall serve exclusively for the purpose of general information. Such articles are not suitable for any (self-) diagnosis and treatment of individual illnesses and medical indications. In particular, they cannot substitute for the examination, advice, or treatment by a licensed physician or pharmacist. No replies to any individual questions shall be effected through the articles.







